ACA Software Helps Ensure Compliance
What Does ACA Compliance Mean for Me and My Employer?
Hello again,
This post is for Applicable Large Employers (ALEs) required to comply with the Affordable Care Act, as well as for their employees. The following was sourced in part from geisinger.org. We hope you find it useful.
For Employees
The Affordable Care Act (ACA) changes the way your employer buys and offers insurance to you and the other employees. Under the ACA, large employers (50 full-time or full-time equivalent employees or more) are required to offer affordable health insurance to their employees.
The ACA states that your employer is also responsible for providing notice to you of the health insurance options they have, including coverage through the Marketplace, and a description of how you may contact the Marketplace for help.
The ACA Health Insurance Marketplace is a platform that offers insurance plans to individuals, families, and small businesses. The Affordable Care Act established the Marketplace as a means to extend health insurance coverage to millions of uninsured Americans.
Employers are required to offer ACA-compliant insurance options to you.
ACA-compliant refers to a major medical health insurance policy that conforms to the regulations set forth in the Affordable Care Act. ACA-compliant individual and small-group policies must include coverage for the ten essential health benefits with no annual or lifetime coverage maximums.
For Employers – Tax Credit Penalties
Federal tax credits are available for low-income individuals and families with an income under 400 percent of the federal poverty level, and are not otherwise eligible for Medicaid. These tax credits are provided on a sliding scale if your employees choose to purchase insurance through the Marketplace. When this occurs, large employers could be penalized.
Since Oct. 1, 2013, businesses with up to 50 employees can purchase coverage through health insurance marketplaces. Since 2016, the marketplaces have been open to employers with up to 100 employees. As a business owner, you can log on to one of the marketplaces, compare the plans for cost and benefits, and assign one to your employees. Your employees must then sign on to the same marketplace and enroll in the product you selected.
Small-business owners with less than 25 full-time equivalent employees with an average annual wage of less than $50,000 qualify for a tax credit. To receive the maximum tax credit, the business needs to have 10 or fewer full-time employees with an average taxable wage of $25,000 or less.
The credit is phased out as the number of full-time employees increases from 10 to 25 and as average employee compensation increases from $25,000 to $50,000. To be eligible, the employer must cover at least 50 percent of the cost of healthcare coverage for their employees.
The amount of the credit is determined by:
- Number of employees – This is determined by totaling all of the employed hours of all employees (part-time and full-time), then dividing that number by 40 (hours per week). If the resulting number is less than 25, your company qualifies for the tax credit.
- Average annual wages.
For tax years 2014 and later, eligible small businesses that purchase coverage through the state Marketplace may receive a tax credit of up to 50 percent of the employer’s contribution toward the employee’s health insurance premium. Employers are eligible to take the tax credit for two years.
Tax-exempt small businesses meeting these requirements are eligible for tax credits of up to 25 percent of the employer’s contribution toward the employee’s health insurance premium for tax years 2010 to 2013, and up to 35 percent for tax years 2014 and later.
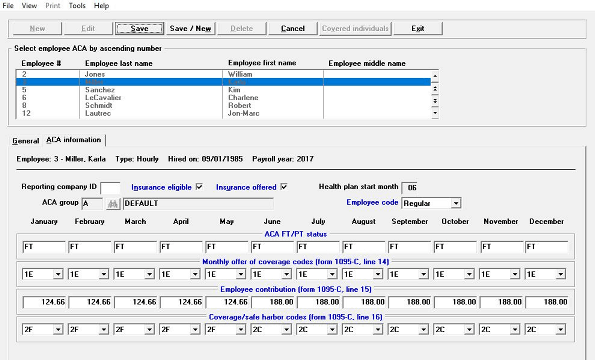
ACA Software
For employers and employees, ACA software can simplify and streamline compliance and reporting. Alerts in easy-to-read reports highlight critical points such as employees who may soon require an offer of qualifying coverage.
High quality ACA compliance software not only handles year end reporting, it helps monitor compliance through the year. Employers can avoid penalties and employees have confidence they are in compliance.
To learn more about Passport Software’s ACA Software or Full Service option call 800-969-7900. Or, contact us – we are here to help.